Introduction
Stress urinary incontinence (SUI) is defined as leakage that occurs during activities that raise intra-abdominal pressure (e.g., coughing, laughing, sneezing, lifting heavy objects). This can range from a few drops to a big gush, if severe.
Normal pelvic and bladder anatomy
The urethra is the tube that drains the bladder to the outside. The bladder and the urethra are supported by layers of muscles and structures (pelvic floor) that lie underneath them. A strong pelvic floor is essential in normal continence; reflex tensioning of the pelvic floor provides counter-pressure to keep the urethra closed, during impact activities.
The sphincter is a ring of voluntary muscle that encircles the urethra. It squeezes tight when one does not want leakage to occur. During voiding, the sphincter relaxes to allow the urethra to open and let urine through.
Mechanisms and causes of SUI
SUI is often due to a combination of urethral hypermobility and intrinsic sphincter deficiency (ISD) in variable proportions.
Urethral hypermobility
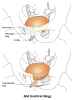
When there is a defect in the supporting pelvic floor, the urethra moves downwards from its resting position during activities such as laughing or coughing, and urine can leak through. This is called urethral hypermobility. Hypermobility-related incontinence implies the bladder outlet is closed at rest and opens during exertion.
Some causes are pregnancy, vaginal delivery, obesity, smoking, chronic cough, chronic constipation, high-impact activity, genes, hysterectomy and certain anti-hypertensive drugs (alpha-blockers).
Intrinsic sphincter deficiency (ISD)
ISD describes a urethral sphincter mechanism that lacks the co-aptation or normal closing pressure needed to prevent exertional leakage. In ISD, the bladder outlet is open at rest and urine can leak through even with lighter impact activities. The most severe form of ISD-related stress urinary incontinence is that of the fixed ‘lead-pipe’ urethra.
Causes include prior surgery, radiation, trauma with scarring or a neurologic condition.
How common is it?
Up to 42% of women in their lifetime will complain of various degrees of stress urinary incontinence.
What other conditions can co-exist with SUI?
- In women who have a concomitant pelvic (vaginal) organ prolapse, SUI may be masked or exacerbated.
- It is quite common for patients to have both SUI and urge incontinence (see overactive bladder) at the same time and this is described as mixed incontinence.
How is SUI diagnosed?
- Assessment would involve a detailed clinical history and, in some patients, a physical examination can be very important. This is always done in the presence of a female chaperone.
- Urinalysis can help rule out an infection as the cause of leakage.
- A bladder diary can quantify the amount of fluid input and leakage. A 24-hour pad weight test can objectively measure the daily volume leaked.
- Urodynamics(bladder function study) is appropriate in patients who are considering surgery to determine the severity of leakage and hence, the best surgical option for that particular patient. Urodynamics can also look for a component of overactive bladder and urge incontinence, which can be improved with medications.
What are the treatments?
Conservative Treatment
- Patients are encouraged to make some lifestyle changes such as losing weight, treating constipation, reducing caffeine intake, and stopping smoking.
- Pelvic floor exercises were first described by Dr Arnold Kegel in the 1940s and they aim to strengthen the pelvic floor muscles and improve bladder neck support. A trained physiotherapist can assist in this.
- Medications are usually not very helpful in treating SUI because the underlying problem is that of an anatomical failure.
Surgical Treatment
Surgical options can be very effective in treating SUI. Surgery has changed a lot over the years with the advent of minimally invasive synthetic (mesh) slings, which have excellent results.
However, in recent years, there has been a move away from synthetic slings due to concerns about mesh implants. As such non-mesh surgery such as the pubovaginal fascial sling is being done more.
Other surgery like the Burch colposuspension is also a non-mesh option, but large studies have shown that it has inferior success rates when compared to the pubovaginal fascial sling.
There are a range of sling types, which differ:
- In the manner that they are positioned (retropubic vs. transobturator and mid-urethral vs. bladder neck).
- In the material that they are made of (synthetic vs. own tissue like fascia).
Mid-urethral sling
The mid-urethral sling or the tension-free vaginal tape (TVT) is made of synthetic mesh material and has excellent long-term results (80% - 90% cure rate at 10 years).
Patients typically stay in the hospital overnight and some can even be discharged on the same day. The sling can be positioned either retropubically (via a route behind the pubic bone) or transobturatorly (via the inner thighs). The surgery involves a 1cm vaginal incision and two other small stab incisions, either in the lower abdomen or in each inner thigh.
Overall complication rates are low and include bladder injury, infection, erosion of the mesh, inner leg pain, incorrect tensioning of the sling, bowel and major blood vessel injuries (rare).
Pubovaginal Fascial sling
This is a non-mesh or mesh-free sling that can be harvested from the patient’s own rectus fascia (layer of tough abdominal wall tissue). Occasionally fascia can also be harvested from a patient’s leg (fascia lata).
The success rates are similar (80% to 90% at 10 years), but the fascial sling has higher morbidity (longer hospital stay, bigger abdominal incision) but lower erosion and infection rates. The fascial sling is placed in a retropubic way – but sits more proximally at the bladder neck as compared to a mid-urethral sling (which is placed in the middle of the urethra). The fascial sling, being a natural sling, may be preferable in some patients especially if there is concern about mesh implants.
A/Prof Gani specialises in this type of surgery. See pubovaginal fascial sling, for more information.
Urethral bulking agents
This involves the injection of bulking agents into the urethra, creating wall-to-wall apposition and hence increasing the outlet resistance. Examples of agents that can be used are collagen (now no longer manufactured), Macroplastique (silicon particles in a viscous gel) and Bulkamid (hydrogel with synthetic polymer).
Success rates are lower at 30 - 50% and the procedure may need to be repeated. It can potentially be done under local anaesthesia and hence is suitable for frail, elderly patients. Some younger patients with mild incontinence who want the least invasive treatment may also prefer this.
Colposuspension
Sutures are placed trans-abdominally to suspend and re-support the bladder neck and vagina to the ligaments on the internal surface of the pubic bone.
The success rate is inferior to a pubovaginal fascial sling and a mid-urethral sling. The long-term success rate is about 70%.
Artificial Urinary Sphincter
The artificial urinary sphincter is more commonly used to treat male stress urinary incontinence that occurs after prostate surgery for prostate cancer (post-prostatectomy urinary incontinence).
In women, it has a role as a salvage option when all other treatments have failed. It is technically a challenging operation with risks of bladder or vaginal wall injury, and therefore it is not commonly done in women. It should not be considered as a primary treatment option as other options are less invasive and have high success rates.
A cuff is placed around the bladder neck, which is connected to a pump that is placed in the labia. These are connected to a balloon reservoir that is placed in the lower abdomen. The cuff encircles the bladder neck and keeps it closed all the time, hence maintaining continence. During voiding, the pump is pressed to open the cuff to allow urine to come through.
Related Information
A/Prof Gani has extensive experience with the pubovaginal fascial sling and is one of the highest volume surgeons in the country doing this.
Read his publication on his technique to achieve the best sling tension with lower risk of complication. He has run workshops and been invited to multiple conferences to give talks on this technique.
Read A/Prof Gani’s publication:
Download Australian national female continence surgery trends over 20 years - PDF (926 Kb)
Read A/Prof Gani’s publication:
Download Surgical mesh information on youtube - PDF (727 Kb)
Read the Australian Commission on Safety and Quality publication:
Download Treatment options for stress urinary incontinence - PDF (589 Kb)